February is famously known as the home of Valentine’s Day and Presidents’ Day, but it’s also less commonly known as American Heart Month and, to those in the optometry realm, Macular Degeneration Awareness Month. Macular degeneration has its own month of awareness for a reason – it’s the leading cause of blindness in the Unites States and is just as prevalent as all forms of cancer combined! Macular degeneration affects more than 10 million Americans and is not talked about as much as it should be, so I’m going to help fill you in on the missing pieces.
What is Macular Degeneration?
It is a disease of the “seeing cells” – your retina, characterized by deterioration of the macula, which is the small spot on the retina (back of the eye) that’s responsible for central vision. The macula is also most sensitive to detail as well as damage. At its worst, you can lose your central vision, rendering you unable to legally drive and at a loss for ease in completing daily tasks.
If you want to get more granular, accumulation of lipid deposits beneath the retina are the root of the problem. The disruption caused by these deposits is characterized by the thinning and drying of the macula. This causes the eye to undergo damage and swelling, which can lead to loss of function of the macula (aka loss of central vision).
Anyone can develop macular degeneration at any age; however, it is most common over 50 years old, in which it is referred to ask age-related macular degeneration, or AMD for short.
Risk Factors:
The three largest risk factors are smoking, a family history of AMD, and uncontrolled hypertension (high blood pressure). Other risk factors include heart disease, being overweight, overexposure to UV light and blue light, old age, pale-colored irises and skin, hyperopia (far-sightedness), and more.
A lot of these risk factors are out of your control, such as: having a family history of AMD, although there are some you do have control over, including smoking, uncontrolled high blood pressure, your weight, and UV and blue light overexposure. It’s extremely important to have regular doctor appointments to get your current health state analyzed to make sure you’re taking steps in the right direction toward a healthier you. If you have high blood pressure, you’ll want to see your doctor about getting it under control with the right medication for you. If you are overweight, you’ll want to start eating healthier, practicing portion control, and exercising – every little step in the right direction helps. Those leafy, green vegetables hold the eye-protecting nutrients we are after. There is an eye vitamin and nutrient pill on the market that is research backed called AREDS 2. Ask us for a free sample today! For more information on what food is good to eat for your eyes, follow this link: https://www.macular.org/good-food
If you spend all day on your phone, tablet, laptop, desktop, tv, or any other device, you should armor up with a pair of blue light blocking glasses. Read our previous blog posts on blue light for more information as to why it’s so harmful: https://theiavisioncare.com/2018/04/17/what-is-blue-light-and-how-can-you-keep-your-eyes-happy-and-healthy/ For UV overexposure, don’t stare into the sun! Hasn’t your mother ever told you that? Also, you should be wearing a pair of quality sunglasses each and every day. That’s right – even in the winter! It’s all about preventing the damage, so being consistent with these things, even when you can’t see the results, is extremely important.
Smoking isn’t just another risk factor – it DOUBLES your risk! My advice to you is to immediately quit. The consequences of smoking far outweigh the benefits. According to the CDC, smoking can cause cancer almost anywhere in your body, and if nobody smoked, 1 in 3 cancer deaths would not occur. For more information on the harmful effects of smoking and what will happen when you quit, follow the link: https://www.cdc.gov/tobacco/data_statistics/fact_sheets/health_effects/effects_cig_smoking/index.htm
For additional eye health tips, read the article at the following link: https://www.macular.org/ten-things-you-can-do-improve-your-vision
Dry Vs. Wet AMD:
As previously stated, macular degeneration is characterized by lipid aggregates accumulating beneath the retinal layer of the eye, causing disruption. When these lipid clumps, called drusen, cause enough disruption, your body sees that there’s a problem and intervenes by growing new blood vessels in attempt to fix it. These weakly-constructed blood vessels are abnormal and very fragile (basically, a bad sign). They’re at high risk for bursting and causing internal bleeding within the eye, which can cause major irreversible damage and vision loss.
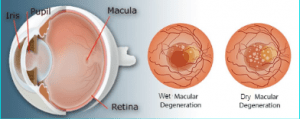
People often confuse the terms “dry MD” and “wet MD” to be different types of the disease, when in reality, they are just different states of the macular degeneration. All MD patients have drusen in their affected eyes, but not all of them have progressed to have leaky blood vessels. Dry MD means you only have drusen in your eye. Wet MD means it has progressed to a bleeding state. View the picture below for help in visualizing the situation.
Treatment:
Macular degeneration is an incurable disease, however, that doesn’t mean there’s nothing we can do to slow down its progression. If your MD progresses to a worse state (wet MD), your doctor may need to take action. Intravitreal injection therapy is an eye injection that inhibits the growth of those fragile, leaky blood vessels. Laser photocoagulation is a surgical procedure in which a laser is used to seal off those dangerous blood vessels. These procedures are not an option if your MD is only dry (drusen only, no leaky blood vessels) because they are more invasive and serious – somewhat of a last resort to save your vision. That’s why you want to control your dry MD as much as possible early on!
Remember, the key in life is prevention! Jump back up to the Risk Factors section and see what you can do today to lower your risk for MD. Ask us more about blue light blockers and come check out our stock of high quality sunnies today!